Health coverage offers families more than the chance to be physically healthy. It also helps to provide financial security. With health insurance comes a sense that you are protected in the case of an unexpected illness or a serious accident. It brings the security of knowing that if something goes wrong with your health or that of your loved ones, you have insurance to help pay the bill.
Today, health insurance is more affordable for millions of Californians. In 2015, 90 percent of Californians received financial assistance in paying for premiums for coverage through Covered California; one in three Californians is enrolled in free or low-cost Medi-Cal. For many, such opportunities have made a world of difference. For other families, having insurance is not enough to remove significant cost barriers, including unaffordable co-payments and deductibles, which prevent them from getting the health care needed to keep their families healthy.
While the proportion of uninsured Californians reporting cost as the reason for lacking coverage fell from 53 percent to 43 percent in 2014, lack of affordability remains the most common reason cited for going without insurance in California. Among people with health insurance, one in five working-age Americans reported having problems paying medical bills in the past year. As a result of these high medical costs, families often end up facing serious financial challenges and may have to face unexpected changes in employment and lifestyle. When insured individuals received medical bills, three-quarters said that the amount they had to pay for their insurance co-payments, deductibles, or coinsurance was more than they could afford. As ACA implementation moves forward, ensuring coverage is affordable for children and their families remains critical to supporting families and creating true peace of mind.
As we live each day, no one ever plans to get sick or hurt, but, inevitably, most people will need medical care at some point in their lives. Health insurance helps cover the cost of the care we need and offers many other important benefits to help us stay healthy. Knowing we are protected is critical to both our physical health and mental health, and it provides that true peace of mind.
Read more about ways coverage can be more affordable in our new report, “The Affordable Care Act and Children’s Coverage in California: Our Progress and Our Future.”
Without a doubt, California has been a leader in health care reform for children and families in more ways than one. When the Affordable Care Act (ACA) was signed into law six years ago, we were the first state in the nation to enact legislation creating a health insurance marketplace—Covered California—offering affordable private insurance options to Californians. Early on, California expanded its Medicaid program to include more low-income adults. To make sure as many children received dental coverage as possible, California embedded dental benefits into the medical benefits package received under Qualified Health Plans in Covered California.
Beyond the reforms included in the ACA, a new group of immigrant children and youth qualified for Medi-Cal coverage in California with the creation of the federal Deferred Action for Childhood Arrivals (DACA) program. Most recently, the State continued to expand its coverage opportunities for those left out of the ACA, namely our immigrant children. As of May 2016, full Medi-Cal benefits are available to all low-income children, regardless of immigration status. A movement that began at the community level has extended statewide, and now all kids have access to coverage across California, the state with the largest immigrant population in the nation.
As more children than ever before have access to health coverage they need and deserve, we must ensure the benefits match their child-specific needs to ensure their healthy development. Quality coverage for kids means a benefits package including child-centered services, such as childhood developmental screenings, hearing aids, and pediatric specialty care. Children with health coverage have better access to needed care, lead healthier lives, and perform better in school.
While coverage eligibility in our country and California is the best it has been in our history, there are still some that remain unable to access affordable insurance. Moderate-income families may be locked out of access to financial assistance for marketplace coverage. Despite the gains made for children, there are still 1.5 million adults in California who remain ineligible for full-scope coverage through Medi-Cal or Covered California due to their immigration status. Fortunately, the Governor recently signed legislation requiring California to seek federal approval to also offer Covered California coverage options to undocumented immigrant Californians, but they would remain ineligible for federal subsidies for their health coverage.
Building on the incredible progress of the ACA will require further federal and state action. At the federal level, some important coverage refinements include:
- Fixing the “Family Glitch,” which refers to how some moderate-income families may be locked out of access to financial assistance for marketplace health plan coverage due to employer coverage that is available yet unaffordable. Federal clarification of the “affordability test” of employer coverage could allow dependents to qualify for marketplace coverage subsidies if the employer’s family coverage is unaffordable.
- Defining the required “pediatric services” category of Essential Health Benefits. ACA requires all Qualified Health Plans to offer a package of Essential Health Benefits, including pediatric services. However, this unique package of benefits has not yet been defined, and states are instead instructed to choose benchmark plans based primarily on employer-based plan packages, which are geared toward adults rather than children. Medicaid’s Early Periodic Screening, Diagnosis, and Treatment (EPSDT) benefit is specifically designed to provide childhood developmental assessments and specific pediatric care, and it serves as a worthy model.
California can continue to be a leader in health care reform for children and their families by taking action on the following:
- Expand Medi-Cal to low-income undocumented immigrant adults and allow undocumented immigrants to purchase coverage through Covered California. When parents are eligible for coverage, the whole family is more likely to enroll and more children can get the health care they need. With the enactment of SB 10, California has the opportunity to allow more Californians the opportunity to purchase health plans through California’s health insurance marketplace.
- Explore affordable coverage options for California families excluded from Covered California subsidies due to the “affordability test.” In the interim, before a federal “family glitch” fix, California could identify coverage options these families can afford. Access to health insurance is important for every Californian and to ensure a healthy future for our children.
- Better define and provide the “Pediatric Services” Essential Health Benefit to youth up to age 21. In lieu of a federal definition of the “pediatric services” Essential Health Benefit, the State should pursue options for offering full child benefits (such as EPSDT) through Covered California for children as a means of providing a sufficient pediatric services benefit package. Also, despite federal regulations stating that states have the flexibility to extend pediatric services coverage beyond the age of 19 and receive federal financial assistance for doing so, California policymakers have yet to exercise this option. Extending to 21 would help more youth receive critical, comprehensive services, including oral and vision care, as they transition into adulthood.
Read more in our new report, “The Affordable Care Act and Children’s Coverage in California: Our Progress and Our Future.”
Today in California and across the country, millions more Americans have access to quality, affordable health coverage. Thanks to the Affordable Care Act, and the tremendous efforts by states, advocates, faith-based organizations, schools, businesses, and communities, including our collaboration with schools through the ALL IN For Health Campaign, more families and children than ever are enrolled in coverage. With coverage, families and children can see a doctor, fill a prescription, and have the peace of mind that health insurance coverage provides—but only if they understand what having an insurance card can mean for them.
Too many people, particularly the newly insured, find health insurance confusing, frustrating, and often overwhelming. For children, their ability to get the care they need depends on their parents’ ability to understand and navigate the coverage system on their behalf. When at least 1 in 3 parents of young children have limited health literacy skills, we know a family’s understanding of health insurance and the health care system will impact a child’s ability to get the care they need.
Part of this understanding is knowing the benefits made available through the ACA and Medi-Cal. A key benefit, for example, is access to preventive services, such as well-child visits, immunizations, and developmental screenings for children, with no additional out-of-pocket costs. Before the ACA, many families, especially minority and low-income families, faced cost barriers that discouraged them from going to the doctor or dentist for a checkup. Instead of going to a primary care doctor to get chronic asthma under control or going to a dental care provider for a cleaning, children ended up in the emergency room with a preventable asthma attack or tooth abscess. Access to regular, preventive health care is a key element to helping all Americans become healthy and stay healthy. Preventive care is particularly critical to children’s development, helping them thrive in school and grow up to become healthy adults. As coverage becomes more widely available, it is time to help families navigate an unfamiliar health care system and ensure that families are using that coverage to get care before health problems arise.
At The Children’s Partnership, we are excited to add this new focus to our ALL IN For Health Campaign and build on our powerful partnership with California schools to educate families about the importance of understanding coverage, including seeking preventive health care. We have developed a new flyer that reinforces the concept of preventive health and gives families four easy steps they can take today to get their families the care they need to stay healthy. To help families keep track of their children’s preventive health visits and other medical information, we’ve also developed a handy card to store key information.
Educating families about how to use their insurance and the importance of preventive services is critical to the well-being of children and their ability to succeed in school. We are excited to continue our work with schools to better the health of California’s students and families and do our part to make sure that the vision of the ACA—a healthier America—becomes a reality.
Share our new flyer, “Get Care: Staying Healthy All Year Round = School Success.”
Order the Get Care Card to distribute to families.
Visit our toolkit to learn more about our new Get Care flyer and Get Care Card.
When I worked at the US Department of Health and Human Services, I was fortunate to travel coast to coast helping educate Latino families about how to enroll in quality, affordable health coverage through the Affordable Care Act. Mothers and tías, fathers and abuelitas would share their stories, their challenges, and their hopes about what the ACA could do for their families. I often talked about my baby sister and how, through the expansion of Medi-Cal, she was able to enroll in coverage and have one more tool to help make sure she can lead a healthy life. Our shared stories reflected the hope we all have for our loved ones—that they be able to lead healthy lives. And since the passage of the ACA, we have made real progress for the future of the Latino community and, in so doing, the state of California.
In California, Latino children make up half of all children under the age of 18. The future of California depends on our ability to ensure their health and well-being. A new report,Historic Gains in Health Coverage for Hispanic Children in the Affordable Care Act’s First Year, shows that the number of uninsured Latino children dropped dramatically in the first year that the ACA took effect, and California led the way, accounting for more than one-third of the national reduction. Released by the Georgetown Center for Children and Families, the National Council of La Raza, and the California Children’s Health Coverage Coalition, the report shows the uninsurance rate for California’s Latino children declined from 9.6 percent in 2013 to 6.8 percent in 2014, a rate significantly lower than the national average of 9.7 percent.
Through the collaborative work of community-based organizations, health centers, churches, promotoras, families, and many others, California made important strides in reaching Latino families and enrolling Latino children. Trusted organizations opened their doors and walked families through the enrollment process. Familiar sources of information shared important details like key dates and answered questions about ways to apply. California opened an incredibly successful marketplace in Covered California and expanded Medi-Cal for adults. In doing so, California provided more children the chance to have coverage, for when parents are enrolled in health insurance, their kids are more likely to be covered.
But despite the progress we have made, we know there is still more work to do. In 2014, California was home to 323,000 uninsured Latino children—the second largest number of any state in the country. Children without insurance are less likely to get the preventive care they need to stay healthy and more likely to face chronic conditions like diabetes or asthma. With a health insurance card in hand, families can take their children to the doctor and dentist on a regular basis, not just when there is an emergency.
Later this year, California will see an expansion of Medi-Cal to include an estimated 170,000 undocumented children. Our state continues to demonstrate leadership as we work to provide every child access to quality, affordable health coverage. In my new role at The Children’s Partnership, I look forward to working with organizations across the state to help get us to 100 percent insurance rate for our future Latino leaders. When we make sure Latino children are covered and healthy, we ensure the future of California is healthy, too.
- Read the report, Historic Gains in Health Coverage for Hispanic Children in the Affordable Care Act’s First Year.
- Read the press release in response by the Children’s Health Coverage Coalition.
- Share at the infographic below by the Children’s Health Coverage Coalition Coalition.
More than a decade ago, The Children’s Partnership teamed up with small business leaders to connect employees and their families to health coverage. While the portion of uninsured children has reduced since that time, workplaces continue to be an important place to engage families with information about how to get their children enrolled in health coverage. One in three uninsured children in California has a parent working for a small business, and many of them are eligible for no- or low-cost health coverage through Medi-Cal or for financial help through Covered California’s individual marketplace. That is why we have rejoined forces with small business leaders in California to make sure families have what they need to connect to care.
Because of certain provisions in the Affordable Care Act (ACA) that take effect this year, this is a critical time when more people, especially those in the small business community, will be paying attention to the legal landscape of how the ACA impacts small businesses and other employers, including the Employer Shared Responsibility Provision and the Small Business Health Options Program (SHOP). While small businesses—those with 49 or fewer full-time employees—are not required to provide health insurance for their workers, Covered California for Small Business can help many employers withfinancial assistance as well as health insurance options. Small businesses with 25 or fewer full-time employees have the opportunity to receive up to a 50 percent tax credit (35 percent for tax-exempt employers). Employers with 10 or fewer full-time employees qualify for the maximum credit. If they do not offer insurance, employers are encouraged to provide information to employees about affordable health coverage opportunities through Covered California and Medi-Cal. Given the important connection they have to eligible families, small business employers need tools and resources to educate their employees about coverage options for the entire
The Children’s Partnership worked with Small Business California, Small Business Majority, Health Law Guide for Business, The California Endowment, and Covered California to develop resources for small businesses to help their employees and families connect to coverage. Please share our flyer and paycheck envelope stuffer with small businesses in your community and encourage them to distribute information.
When children have health coverage, it benefits children, parents, and employers alike! Studies show that when children have health insurance, their parents are less stressed, miss fewer days of work, and are more productive.
If you act now, you can help connect families to coverage before Covered California’s open enrollment ends on January 31. There are also plenty of opportunities to connect individuals to health coverage year round through Medi-Cal, and eligible individuals can enroll in Covered California anytime if they experience a qualifying life event, such as having a baby, getting married, or moving.
Share this link with small businesses you know in your community: www.childrenspartnership.org/smallbusinessforkidshealth.
Learn more about TCP’s strategy.
Download the flyer for small businesses (English and Spanish).
Download the paycheck envelope stuffer for small businesses (English and Spanish).
Download the briefing document, “Connecting California Children to Health Coverage Through Small Business.”
We are now in the midst of the third open enrollment period for Covered California, the state’s marketplace for affordable health coverage options. And schools and early learning centers across California are once again at the forefront working to inform families about the opportunity to enroll in coverage. Using The Children’s Partnership’sALL IN For Health toolkit, schools and early learning sites are making calls, passing out flyers, sending newsletters, sharing social media messages, and, ultimately, connecting families to enrollment assistance.
But after a successful first two years of enrollment, what should schools and other outreach partners be focused on this year? Based on the research, we know there are some top points to emphasize to make sure kids and their families get covered and stay covered:
- Financial Help Can Lower Monthly Costs: A recent Covered California survey showed that many uninsured individuals who can benefit most from affordable coverage options still do not understand that they can get financial help to lower monthly costs. Therefore, we need to focus our messages on the premium subsidies available through Covered California and the fact that Medi-Cal is free or very low cost. On the flip side, it is also important to remind families that if they don’t get coverage, they might have to pay a fine of $695 per person or 2.5 percent of their income—whichever is greater.
- Enrollment Help Is Available: Studies after previous enrollment periods demonstrate that many people seeking health coverage prefer to talk with someone who can help them understand their coverage options. ALL IN can arrange for Certified Enrollment Counselors who speak English, Spanish, and potentially other languages to be available on site—such as at schools or early learning centers to walk families through the enrollment process and ensure they enroll.
- Shop Around and Renew Every Year: Each year there are new plans and new prices available. Everyone is encouraged to shop the health coverage marketplace during open enrollment and ensure they have the plan that best meets their family’s needs and budget, especially if the family has had any changes in income. For those with coverage through Covered California that are satisfied with their coverage, they will be automatically re-enrolled in their health plan. Medi-Cal will mail renewal packets each year, and families must respond to keep their coverage.
These are just a few messages schools and early learning providers can spread to make this third year of open enrollment as successful as possible. If you have additional ideas on what to focus on or would like to partner with the ALL IN For Health Campaign, please contact us.
Download resources from The ALL IN For Health Fall 2015 Toolkit.
Covered California open enrollment is November 1, 2015, to January 31, 2016. Medi-Cal enrollment is available all year long. Apply through www.coveredca.com.
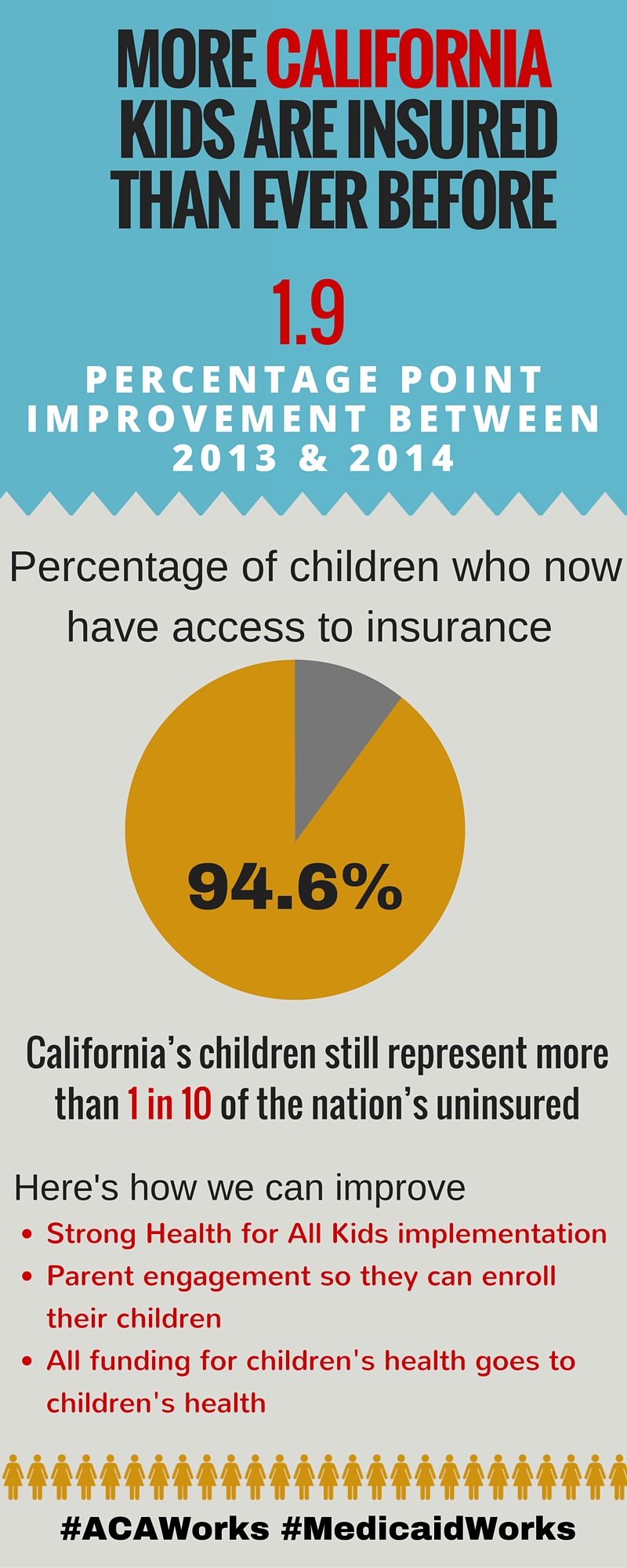
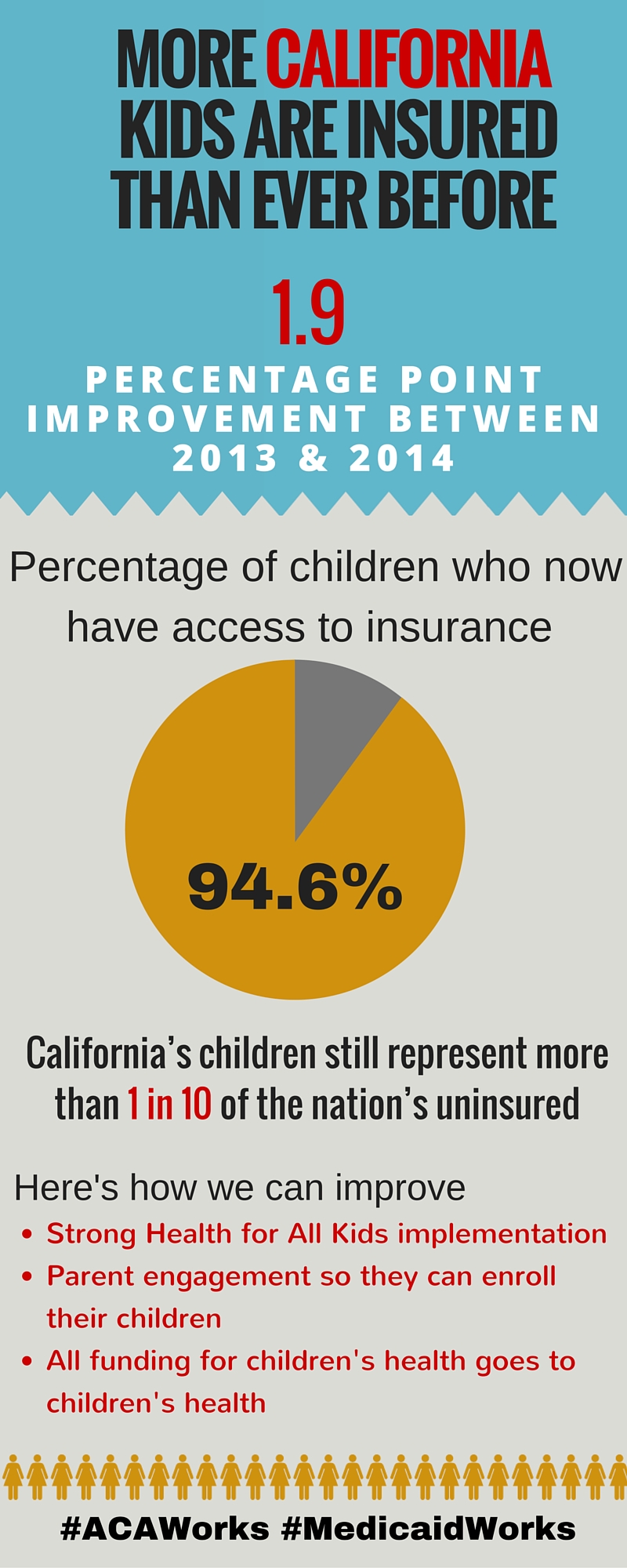
As we begin the third Covered California open enrollment period, we now have new data to show how well we have done so far in reducing the number of uninsured children in California. The new report, released jointly by Georgetown University Center for Children and Families and the California Children’s Health Coverage Coalition, shows that 176,000 fewer children in California were uninsured in 2014 compared to 2013. That 1.9 percent drop amounts to a statewide uninsurance rate of 5.4 percent compared to 6 percent nationally.
Many of the improvements in children’s coverage rates can be attributed to new coverage opportunities for children through Covered California as well as the Medi-Cal expansion for adults and the continued success of Medi-Cal in meeting the health coverage needs of uninsured children and families. Of note is that the Medi-Cal expansion for parents led to more children enrolling in Medi-Cal coverage, known as the “welcome mat” effect—when parents are eligible for coverage, they are more likely to enroll their eligible children. The increase in coverage is also a result of forward-thinking approaches to simplifying enrollment for eligible individuals. For example, Express Lane Enrollment, a streamlined enrollment process into Medi-Cal for those who are already enrolled in the Supplemental Nutrition Assistance Program (SNAP, formerly the Food Stamp Program), led to hundreds of thousands of adults and children being automatically enrolled in Medi-Cal health coverage because they were enrolled in SNAP.
Committed state leaders are to thank for these great strides in connecting California children and families with the health care opportunities made available by the Affordable Care Act (ACA). At The Children’s Partnership, we’ve also seen education leaders step up and connect students and families to health coverage through our ALL IN For Health Campaign. Through partnerships with education leaders and others, our collective efforts enable us to reach families where they are and connect children to coverage, improving their ability to succeed academically and stay on track developmentally so they can achieve their full potential.
But we still have more to do. California ranks 29th nationally when it comes to kids’ coverage, and there are still about 497,000 uninsured children in California, most eligible for Medi-Cal but not enrolled. This Covered California open enrollment period, and throughout the year for Medi-Cal, we can continue to focus on enrolling these remaining uninsured kids.
We also now have an opportunity to do even more for children in the implementation of Health for All Kids—which will provide Medi-Cal coverage to over 170,000 children who did not previously qualify. Beginning as early as May 1, 2016, all income-eligible children, regardless of immigration status, will be eligible for Medi-Cal. It’s up to us to ensure we make enrollment for these children as smooth and expedient as possible, and TCP will work with the State to help make that happen.
The Children’s Partnership will continue to partner nationally with Georgetown CCF and in California with the Children’s Health Coverage Coalition—which also includes California Coverage and Health Initiatives, Children Now, Children’s Defense Fund-California, PICO California, and United Ways of California—to promote and enhance the Affordable Care Act for kids.
Read the story in Public News Service.
Open enrollment in the state’s health coverage marketplace, Covered California, is available from November 1, 2015–January 31, 2016. Medi-Cal enrollment is available year round. Apply at coveredca.com.
Originally Posted in Say Ahhh! A Children’s Health Policy Blog
By Sonya Schwartz
Now Playing: Coverage for more than 400,000 children and youth
Coming Soon: Coverage for more than 800,000 additional immigrant children, youth and parents
This week, Georgetown University’s Center for Children and Families and The Children’s Partnership released a new paper outlining how to get ready for big coverage opportunities in California. It highlights opportunities that will provide coverage to more than a million people in California’s immigrant families when immigration relief takes affect.
But as spelled out in the paper, Immigration Relief for Parents and Youth = Whole Family Health Coverage in California, while we wait for some of the immigration relief-related coverage options in California to become available, there is a lot that advocates and community organizations in California can do right now to cover eligible children and youth in immigrant families. Here is the run down of coverage opportunities “now playing” in California and also “coming soon” that could get many more children, youth and parents in immigrant families covered.
Now Playing: More than 400,000 children in immigrant families are already eligible for full scope or state-funded Medi-Cal but are not yet enrolled. It is not too soon to roll up our sleeves and get to work on covering them. Here’s the breakdown:
- More than 200,000 youth who qualify for the 2012 DACA program are estimated eligible for Medi-Cal but not yet enrolled. The initial DACA program announced in 2012 is for youth who came to the US before their 16th birthday; have continuously lived in the US since January 15, 2008; are at least 15 years old; are currently enrolled in school or qualifying adult education; or have graduated or obtained a certificate of completion of high school. Our estimates show that of the 343,000 youth qualified for the 2012 DACA program in California, 60 percent or 206,000 are uninsured and eligible for state-funded Medi-Cal. Not all of these 343,000 youth have applied for or been granted DACA status, but if they do receive DACA status and meet the income requirements, they are eligible for a state-funded version of Medi-Cal.
- More than 200,000 citizen or lawfully residing children in immigrant families are eligible for Medi-Cal but not yet enrolled. Our estimates show that 1.6 million children are living with immigrant parents who will be eligible for the new DAPA program in California. DAPA was announced on November 20, 2014, and, when implemented, will allow undocumented immigrant parents who have U.S. citizen or lawful permanent resident children, to apply for work authorization and protection from deportation, if the parent has been in the U.S. since January 1, 2010. Of those 1.6 million California children in DAPA families, 14 percent or 223,000 children are currently eligible for full scope Medi-Cal but remain uninsured. Reaching and enrolling these 223,000 children living in DAPA families would make a huge dent in the number of California’s uninsured children. This map shows that most of these DAPA families live in Southern California with the greatest concentration in Los Angeles County, followed by Orange County, San Diego County, Riverside County, and San Bernardino County.
Coming Soon: There are also opportunities to provide health coverage to more than 800,000 additional immigrant children, youth, and parents and the time to prepare is now. California just passed a law that will provide coverage to all children regardless of immigration status. And, when Deferred Action for Parents of Americans and Lawful Permanent Residents (DAPA) the 2014 expanded Deferred Action for Childhood Arrivals (DACA) program take effect, hundreds of thousands of children, youth, and parents will be eligible for state-funded Medi-Cal. People granted DAPA or DACA statuses are not eligible for federal matching funds for Medicaid or CHIP or for federal premium tax credits in the health insurance marketplace. However, California provides state-funded Medi-Cal coverage for persons residing under color of law (or PRUCOLs), and DACA grantees.
- 170,000 children in California will be eligible for state-funded Medi-Cal for children regardless of immigration status. California recently passed a budget bill (SB 75) that includes health coverage for all children up to 266 percent of the federal poverty level, regardless of immigration status. Children will enroll in a state-funded version of Medi-Cal and coverage will begin no sooner than May 2016. The expansion is estimated to cover 170,000 children.
- More than 600,000 parents in California will qualify for DAPA and likely to be eligible for state-funded Medi-Cal if granted DAPA status. More than 1 million parents in California are estimated to qualify for DAPA and 56 percent are low income by Medi-Cal standards and lack health insurance.
- More than 50,000 youth in California will qualify for the 2014 expanded DACA program and are likely to be eligible for state-funded Medi-Cal if granted DACA status. The expanded DACA program, announced on November 20, 2014, but on hold because of litigation, is also for youth who came to the US before their 16th birthday but who have continuously lived in the US since January 1, 2010 and meet other requirements. Estimates show that of 92,000 youth qualified for expanded DACA, 60 percent or 55,200 are uninsured and likely eligible for state-funded Medi-Cal.
If you are a children’s or immigration advocate or social service provider in California, our paper also provides specific suggestions about what you or your organization can do to help get children, youth, and parents in immigrant families covered. If advocates, service providers, and others working on health care, immigration, and child and family well-being work together to educate and enroll children and families in health insurance, it could lead to a significant reduction in California’s uninsured rate.
State-funded Medicaid coverage for DAPA and DACA grantees and the new coverage opportunity for children regardless of immigration status is unique to California and a few other states. But, all states cover citizen children in immigrant families. And, the majority of other states (twenty-eight) provide coverage to lawfully residing children in immigrant families. Although, there is always more work to be done get these eligible children enrolled in health coverage.
Continue reading on the Georgetown Center for Children and Families website.
Today marks 50 years since Medicaid was signed into law and it is truly a day to celebrate. The program has had a long, successful history of bringing health care to children and families most in need. A combined federal-state effort to finance health programs and ensure timely care, Medicaid provides coverage for nearly 33 million children, or 37 percent of all children living in the United States. All of these children are able to get regular preventive care, from well-child visits and immunizations to dental, hearing, and vision care. And Medicaid provides services for children with special health care needs as well.
Now that longitudinal data is available, we can squarely say that the benefits of providing health care go far beyond the doctor’s office. In honor of the occasion, our partners at The Georgetown Center for Children and Families released a report detailing the growing body of research that shows the long-term benefits Medicaid has provided to children and the nation. Children with access to Medicaid are proven to have better health as adults, with one study showing a 26 percentage point decline in the incidence of high blood pressure in adulthood. Enrollment in the program is also associated with greater academic achievement and higher likelihood of graduating from high school and college. And recent studies suggest that giving low-income kids access to health coverage boosts their future earnings for decades, therefore increasing their future income tax contributions and helping generate an even bigger return on investment.
California is leading the way in giving families peace of mind, knowing that their children have health coverage that allows them to be healthy and productive. Thanks to recent action, starting no sooner than May 2016, California will cover the last remaining group of uninsured children—those who are undocumented. This will ensure more kids in the state than ever before can get a fair shot in life and will help reduce California’s still-unacceptable 7.4 percent children’s uninsurance rate in the state.
In California, and across the nation, we need to continue to both protect and expand Medicaid. The benefits to children’s health, education, and long-term prosperity could not be clearer. On the fiftieth anniversary, let’s commit to keeping Medicaid strong for future generations of children.